Neuroplasty
Neuroplasty (or Epidural Adesiolysis)
After any injury or inflammation or back (spinal) surgery, scar tissues usually form. Even a slipped disc can irritate the surrounding tissues and cause adhesions or scarring. Excessive scar tissues may press into the nerve, causing inflammation and pain.
Neuroplasty (Epidural Adhesiolysis) is a procedure to remove pressure caused by excessive scar tissues in the epidural space. The epidural space is a thin area between the inside of the spine (disc) and the protective layer around the spinal cord.
How is Neuroplasty Performed?
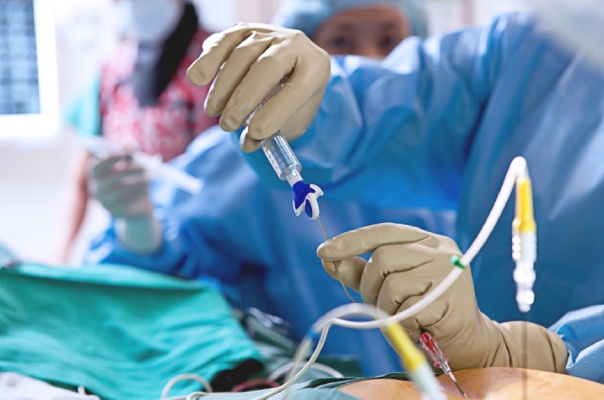
Neuroplasty is similar to the ballooning of blocked heart vessels done on patients with heart problems. You will be given local anaesthesia with mild sedation. Then, you will be asked to lay on your stomach for the procedure. The physician will perform the procedure under X-ray guidance that provides a look into the spine. Following that, contrast dye will be injected to highlight the area affected by the scar tissue. A tube (catheter) will then be inserted, from which a mixture of medicine will be administered to decrease the swelling and relieve the pain.
If necessary, a balloon may be inserted to create more space around the compressed nerves. The physician may also use pulsed radiofrequency to encourage nerve regeneration if needed.
Who will benefit from Neuroplasty (or Epidural Adesiolysis)?
Patients with the following conditions will benefit from Neuroplasty:
- Chronic lower back and leg pain
- Spinal Stenosis
- Patients who had prior back/neck surgery but still have persistent pain
- Patients with herniated disc that is not surgically correctable
- Patients who do not want surgery
- Patients with high surgery risk
Is there downtime? What are the risks and side effects?
Neuroplasty is done as a day-surgery procedure, under local anaesthesia. It is relatively low-risk, with a short recovery time. Generally, patients can go home within the same day.
What is recovery like?
Neuroplasty (or Epidural Adesiolysis) is a day-surgery procedure. The patient can go home on the same day and, the next day, patient can get back to work or to their daily activities. The anaesthesia in the legs may last for 24 hours. The patient will not need long duration of rest in bed. Once the anaesthesia wears off, the patient may feel a different type of ache. The original pain may disappear immediately or go off in a few weeks. It is similar to having a dental procedure. There is no down-time to this procedure. After the procedure, the patient would need to start a rehabilitative programme to work and strengthen the surrounding muscles. There would be some medications (not pain killers) to stabilize the surrounding nerves to make them less irritative.
Is the pain relief permanent?
Most of the patients would have long term relief of 2 years or more. This procedure is similar to ballooning of the heart vessels. If the catheter is able to pass over the narrowing of the spinal canal, the outcomes would be good. However, patients will continue to degenerate, and wear-and-tear will happen. A new area of pain can occur either in a different part or in the same part of the spine. This procedure is usually carried out together with nucleoplasty to improve the overall outcome.
What are the risks and side effects?
There are almost no risks or complications. The procedures are done under the vision of the Xray, which delineates the safe and unsafe zones. This is 99% safe, without any risk of paralysis. There is less than 0.5% chance of nerve injury, infection or bleeding. The procedure is much less invasive than the traditional open surgical approach.



