Nucleoplasty
Nucleoplasty (Percutaneous Disc Decompression) is a minimally invasive procedure to decompress a herniated disc in the spine that may irritate nearby nerve roots. This will reduce the disc protrusion and also reduce the pressure caused by the compression of the nerve roots or the spinal cord.
The minimally invasive procedure is done using coblation (controlled ablation) technology. Coblation utilises low-temperature radio-frequency energy to dissolve tissues in the centre of the spinal disc. Once the excess disc is “vaporized”, it will cause a vacuum effect within the disc, causing the herniated disc to shrink back in. This technology minimizes the risk.
How is Nucleoplasty Performed?
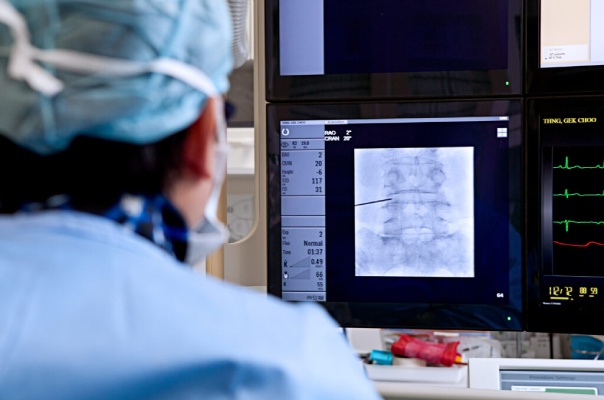
First, a small needle is placed in the centre of the disc. An X-ray will be used to accurately locate the needle inside the affected disc, followed by injection of a contrast dye to provide more visibility. A wand-like coblation device will then be placed through the needle to generate radio frequency energy that vaporizes and removes excess tissues. This reduces most of the pressure to the neighbouring nerves. This procedure is done as a day-surgery, with very low incidence of complications and a short recovery period.
Who will benefit from Nucleoplasty?
Nucleoplasty is suitable for patients with the following conditions:
- Pain caused by a bulging or herniated spinal disc, causing lower back pain that may radiate to the legs
- Spinal stenosis
What is recovery like?
Nucleoplasty is a day-surgery procedure. The patient can go home on the same day and, the next day, patient can get back to work or return to their daily activities. The patient does not need a long duration of rest in bed. Once the anaesthesia wears off, the patient may feel a different type of ache. The original pain may disappear immediately or goes off in a few weeks. It is similar to a dental procedure.
Is there any downtime?
There is no down time to this procedure. After the procedure, the patient would need to start a rehabilitative programme to work and strengthen the surrounding muscles. There would be some medications (not pain killers) to stabilize the surrounding nerves to make them less irritative.
What are the risks and side effects?
There are almost no risks or complications. The procedures are done under the vision of the X-ray, which delineates the safe and unsafe zones. This is 99% safe, without any risk of paralysis. There is less than 0.5% chance of nerve injury, infection or bleeding. The procedure is much less invasive than the traditional open surgical approach.
Is the pain relief permanent?
Most patients will have permanent relief. This procedure is similar to micro-discectomy – an open surgery to remove the excess herniated disc. However, patients will continue to degenerate, and wear-and-tear will happen. A new area of pain can occur either in a different part of the same part of the spine.



